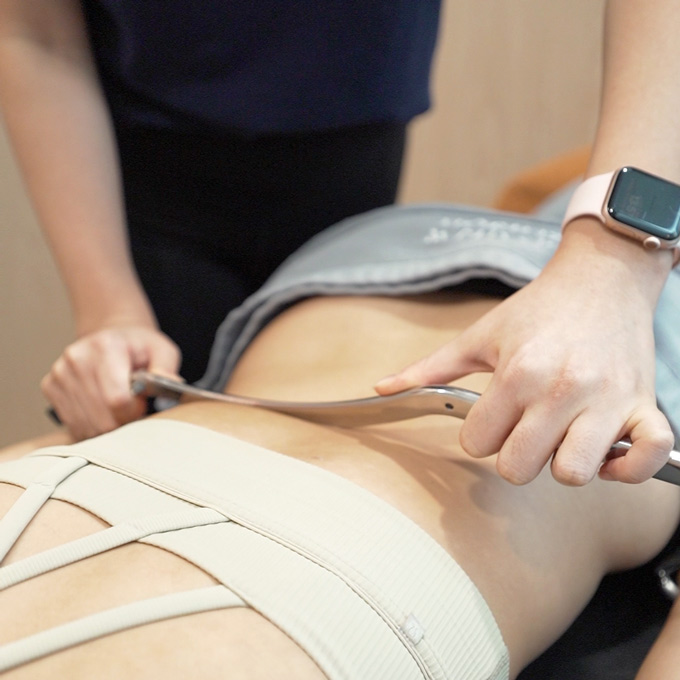
Women’s Health and Physiotherapy
Women experience many physical changes throughout different life stages, including adolescence, pregnancy, postpartum recovery and menopause. These changes can affect the muscles, joints, pelvic floor and overall body mechanics, sometimes leading to pain or functional issues. Women’s health physiotherapy focuses on managing musculoskeletal and pelvic health conditions specific to women. Through detailed assessment and personalised treatment plans, physiotherapists help improve pain, restore function and support long-term health. At MOBILIZE, we provide one-on-one physiotherapy assessment and treatment to support women through pregnancy preparation, prenatal care, postnatal recovery and long-term pelvic and core health.
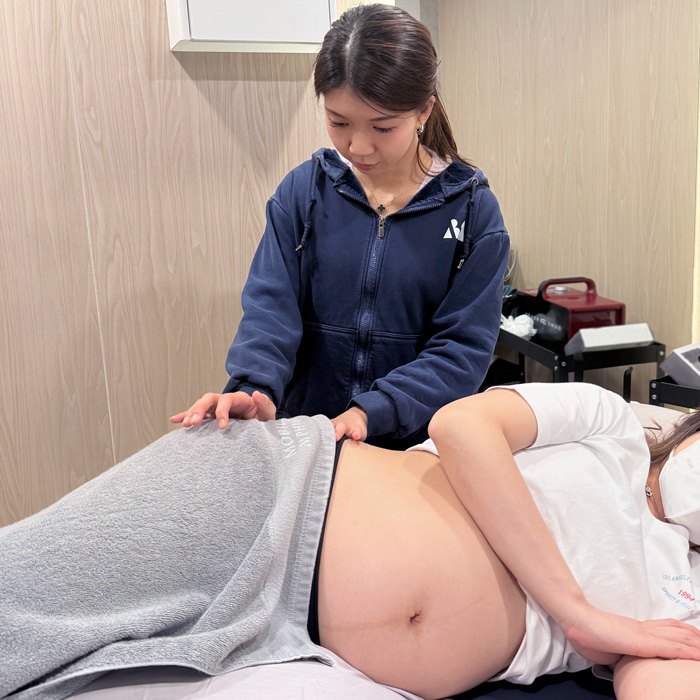
Prenatal Physiotherapy
Pregnancy is an exciting journey, but as the body undergoes structural and hormonal changes, many women may experience varying degrees of physical discomfort during this period. Common symptoms include lower back pain, pelvic girdle pain, lower abdominal discomfort, and muscle tension related to postural changes. Some women may also experience pregnancy-related headaches or swelling, which can affect daily activities and sleep quality.
The goal of prenatal physiotherapy is to help expectant mothers safely maintain mobility and physical function while reducing common pregnancy-related discomforts. Through a professional assessment, physiotherapists provide personalised exercise recommendations based on each individual’s condition. These may include pregnancy-safe stretching exercises, core stability training, and posture modification for daily activities. Appropriate prenatal exercise not only helps reduce pain and discomfort, but also supports overall physical fitness during pregnancy and prepares the body for labour and postnatal recovery.
Common Pregnancy Pain: Back Pain, Hip Pain, Swelling & Headache
Pregnancy Back Pain & Hip Pain
Back pain and hip pain are among the most common musculoskeletal complaints during pregnancy. As the abdomen grows, the body's center of gravity shifts forward, increasing the load on the lumbar spine and pelvis. Hormonal changes can also cause ligaments and joints to become more relaxed, which may reduce stability around the pelvis and hip joints. As a result, many pregnant women experience lower back pain, hip discomfort, or pelvic girdle pain, especially when walking, standing for long periods, or turning in bed.
Pregnancy Swelling (Edema)
Swelling during pregnancy, also known as edema, is a common condition, particularly in the later stages of pregnancy. Hormonal changes, increased blood volume, and the growing uterus may place pressure on blood vessels, leading to swelling in the feet, ankles, and lower legs. Prolonged sitting, standing, or reduced physical activity may further worsen swelling. Appropriate exercises, circulation-promoting movements, and posture advice from a physiotherapist can help improve blood flow and reduce pregnancy-related swelling.
Pregnancy Headache
Some women may experience headaches during pregnancy. These headaches can be related to hormonal changes, poor sleep quality, increased stress, or tension in the neck and shoulder muscles. Postural changes during pregnancy may also lead to increased strain on the cervical spine and surrounding muscles. Physiotherapy can help manage pregnancy-related headaches through posture assessment, manual therapy, muscle relaxation techniques, and appropriate exercise recommendations.