That sharp, stabbing heel pain with your first steps in the morning is a common complaint among many people in Hong Kong. Whether you’re rushing to the MTR, walking up steep hills, or standing for long hours at work, heel pain can quickly disrupt daily life.
In most cases, the underlying cause is Plantar Fasciitis — a condition involving excessive strain and degeneration of the plantar fascia — and it is frequently associated with the biomechanics of Flat Feet (Pes Planus).
At our Hong Kong physiotherapy clinic, we see firsthand how plantar fasciitis and flat feet are closely linked. This guide provides an evidence-based, physiotherapist-led explanation covering anatomy, risk factors, diagnosis, and modern treatment strategies to help you understand and resolve morning heel pain effectively.
Table Of Content
The Anatomy of Pain: What Is the Plantar Fascia and Why It Causes Heel Pain
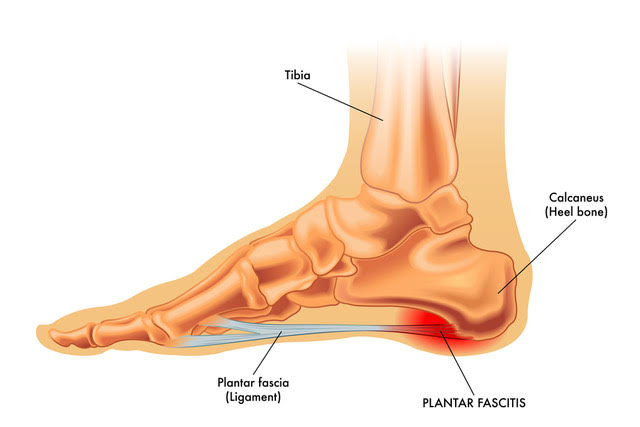
The plantar fascia is a critical structure. It is a thick, fibrous band of connective tissue, one of the strongest in the body, that runs along the bottom of your foot. Think of it as a bowstring supporting the arch of your foot (the “bow”).
- Origin: It attaches to the heel bone (calcaneus).
- Insertion: It fans out forward to attach to the base of all five toes.
- Primary Function: It supports the foot’s arch, absorbs impact when you walk or run, and, through the “windlass mechanism,” helps stiffen the foot for an efficient push-off. When this mechanism is stressed by a flat foot, pain begins.
Plantar Fasciopathy: More Than Just "Inflammation"
Modern research shows this condition is often a degenerative fasciopathy, meaning the tissue breaks down from chronic overuse and repetitive micro-tears rather than a simple acute inflammation. This explains why it can be so persistent and why rest alone is often not enough.
Recognizing the Symptoms: Is It Plantar Fasciitis?
Classic Symptoms of Plantar Fasciitis:
- First-Step Pain: The hallmark symptom is intense heel pain upon waking.
- Pain with Prolonged Activity: Pain may subside after moving, then return after long periods of standing or walking.
- Tenderness: Specific tenderness on the inside-bottom of the heel.
- Stiffness: Often accompanied by tightness in the calf or Achilles tendon.
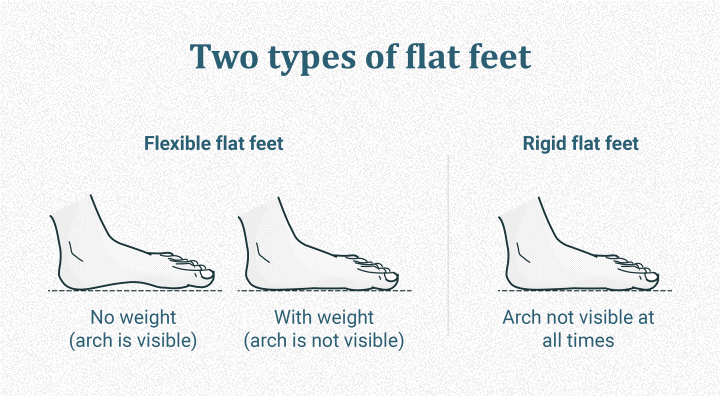
Flat feet are characterized by a collapse of the medial longitudinal arch when standing. This can be:
- Flexible Flatfoot: The arch appears when sitting (non-weight-bearing) but flattens when standing. This is most common and highly relevant to plantar fasciitis.
- Rigid Flatfoot: The arch is absent in all positions, often due to bony issues, requiring different care.
Understanding your risk factors is the first step in prevention. If several of these apply to you, your likelihood of developing plantar fasciitis increases significantly:
- Foot Biomechanics: Having flat feet (pes planus) or, conversely, very high arches (pes cavus). Both alter load distribution.
- Occupational & Lifestyle Factors: Prolonged standing or walking on hard surfaces is a major risk. Think retail workers, teachers, nurses, and hikers on Hong Kong’s many paved trails.
- Physical Activity & Training Errors: A sudden increase in activity intensity, duration, or frequency (like starting a new running regimen on Bowen Road). Repetitive impact sports like running, basketball, and dance are common triggers.
- Age and Weight: The condition is most common in individuals between 40 and 60, as tissue elasticity decreases. Excess body weight (BMI > 27) dramatically increases strain on the plantar fascia.
- Muscular Tightness & Weakness: Chronic tightness in the calf muscles (Achilles tendon) and weakness in the foot intrinsic muscles, ankles, or hips are primary biomechanical causes we treat daily.
A correct diagnosis is crucial. A physiotherapist conducts a thorough assessment, which typically includes:
- Physical Exam: Checking foot posture, arch height, ankle alignment, and palpating for tenderness.
- Functional Tests: Like the “Windlass Test” (dorsiflexing the big toe) to reproduce heel pain.
- Gait & Movement Analysis: Observing how you walk, run, or squat to spot abnormal mechanics that start from the hip or knee.
- Strength & Mobility Tests: Assessing calf flexibility, hip strength, and ankle range of motion to find the root cause.
The Critical Biomechanical Link: Why Flat Feet Lead to Plantar Fasciitis
The connection is rooted in mechanics and supported by research.
- The Biomechanical Problem: A flat foot over-pronates (rolls inward excessively) when you bear weight. This places constant, excessive tension on the plantar fascia as it struggles to support the unstable, collapsed arch.
- Research Evidence: Studies confirm this link. A 2018 study in the Journal of Orthopaedic Research found individuals with flat feet had significantly thicker plantar fascia (a sign of chronic strain). A 2023 study in Gait & Posture highlighted that patients with both conditions exhibited significantly weaker plantar flexor and hip muscles than those with plantar fasciitis alone, showing the problem often extends up the kinetic chain.
In short, the flat foot creates a faulty foundation, and the plantar fascia is the overworked structure that painfully fails under the strain.
Evidence-Based Physiotherapy for Plantar Fasciitis and Flat Feet: A Two-Phase Approach
Our treatment philosophy at Mobilize Physio tackles both the painful symptoms and the underlying mechanical cause to prevent recurrence.
Phase 1: Pain & Tissue Healing
- Shockwave Therapy: A leading evidence-based treatment for chronic plantar fasciitis. It uses sound waves to stimulate the body’s natural healing processes, break down scar tissue, and reduce pain. Studies show high success rates, especially for cases lasting over 6 months.
- High-Energy Laser Therapy: Uses specific light wavelengths to reduce inflammation and promote cellular repair deep within the fascia.
- Manual Therapy & Dry Needling: Hands-on techniques and precise needling to release tension in tight calves, foot muscles, and the plantar fascia itself, reducing immediate strain.
Phase 2: Correcting Mechanics & Building Strength (The Key to Long-Term Success)
This phase directly addresses the research findings on weakness and is essential for lasting relief.
- Targeted Exercise Prescription:
- Foot Intrinsic Strengthening: Exercises like “short foot” or towel scrunches to rebuild your active arch from within.
- Calf & Hip Strengthening: To control the forces transmitted from the ground to your foot.
- Stretching Protocols: Consistent calf and plantar fascia stretching (e.g., using a fascia fighter or rolling a cold bottle).
- Gait Retraining: Teaching you to walk or run in a way that minimises pronation and strain.
- Supportive Strategies & Education: We provide temporary taping for arch support and evidence-based advice on footwear. While custom orthotics can be an excellent supportive tool, our goal is to use them as a bridge while we build your body’s natural, muscular support system.
What You Can Do: Immediate Self-Management Tips
While professional care is key, you can start today:
- Roll and Stretch: Roll your foot over a frozen water bottle for 5-10 minutes, followed by a sustained calf stretch.
- Supportive Footwear: Avoid walking barefoot at home. Wear shoes with good arch support from the first step out of bed.
- Modify Activity: Temporarily reduce high-impact activities like running and jumping. Switch to swimming or cycling.
Frequently Asked Questions
A: Mild cases may improve, but persistent symptoms often require physiotherapy to correct the underlying biomechanical causes and prevent recurrence.
A: Not always, but flat feet significantly increase strain on the plantar fascia, especially when combined with muscle weakness or prolonged standing.
Conclusion: Your Path to Pain-Free Mornings Starts Here
Living with heel pain in Hong Kong’s demanding environment is not something you have to accept. Plantar fasciitis linked to flat feet is a treatable mechanical problem. Success lies in a precise diagnosis and a rehab plan that strengthens your body’s foundation.







Physiotherapy Service
Mobilize Physio is a physiotherapy center located in Hong Kong. Our team of professional physiotherapists provides high-quality, evidence-based pain treatment. Our services include sports injury treatment, pain management, post-surgery rehabilitation, and posture and body alignment correction.
Every patient is unique, and we believe that every treatment plan should be customized accordingly. Therefore, we focus on one-on-one service to ensure that each patient receives personalized attention and specialized care. Contact us today to learn more about our physiotherapy services.
Latest Blog Posts

Conquering Morning Heel Pain in Hong Kong: The Deep Link Between Flat Feet & Plantar Fasciitis

SCHK Marathon Injury Survival Guide: 7 Common Running Injuries, Self-Management & Physiotherapy

SCHK Marathon Injury Prevention Survival Guide: Taping Tips & Physio Secrets for Hong Kong Runners

What Is Shockwave Therapy? A Non-Invasive Solution for Musculoskeletal Pain

ACL Tear: Do You Need Surgery Immediately? Why Prehab & Proper Rehab Matter More Than You Think

Foot Care for Trailwalker & Ultra-Endurance Events: Prevent Injuries, Boost Performance